Distribution of blood flow and ventilation in the lung: gravity is not the only factor. Anatomy and physiology of the airway circulation. Effect of inspiratory flow rate on regional distribution of inspired gas. Distribution of blood flow and ventilation-perfusion ratio in the lung, measured with radioactive carbon dioxide. Regional distribution of inspired gas in the lung. Milic-Emili J, Henderson JAM, Dolovich MB, et al. Transition from dynamically maintained to relaxed end-expiratory volume in human infants. Mechanisms determining residual volume of the lungs in normal subjects. Cellular adaptations in the diaphragm in chronic obstructive pulmonary disease. In: Crystal RG, West JB, Weibel ER, Barnes PJ, editors. Skeletal muscle properties: diaphragm and chest wall. Modulation of neurotransmission in airways. Muscarinic receptors, characterization, coupling and function. In: Crystal RG, West JB, Barnes PJ, Weibel ER, editors. The 2008 Carl Ludwig Lecture: retrotrapezoid nucleus, CO 2 homeostasis, and breathing automaticity. Neuromuscular structure and function in the airways. Pulmonary immunobiology and inflammation in pulmonary diseases. Comparison of planar and tomographic gamma scintography to measure the penetrating index of inhaled aerosols. Phipps PR, Gonda I, Bailey DC, Borham P, Bautovich G, Anderson SD. Involvement of upper-airway muscles in extrapyramidal disorders. Vincken WG, Gauthier SG, Dollfuss RE, Hanson RE, Darauay CM, Cosio MG. The role of inspiratory dynamic compression in upper airway obstruction. Particle deposition in the human respiratory tract. Measurement of tracheal and bronchial mucus velocities in man: relation to clearance. Philadelphia, PA: Churchill Livingstone 2003. Anatomy and physiology of the respiratory system and the pulmonary circulation. Factors affecting upper airway resistance in conscious man.
Pressure-diameter relationships of the upper airway in awake supine subjects.

Wheatley JR, Kelly WT, Tully A, Engel LA. Palate and hypopharynx – sites of inspiratory narrowing of the upper airway during sleep. This process is experimental and the keywords may be updated as the learning algorithm improves. These keywords were added by machine and not by the authors.
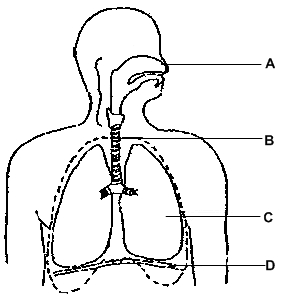
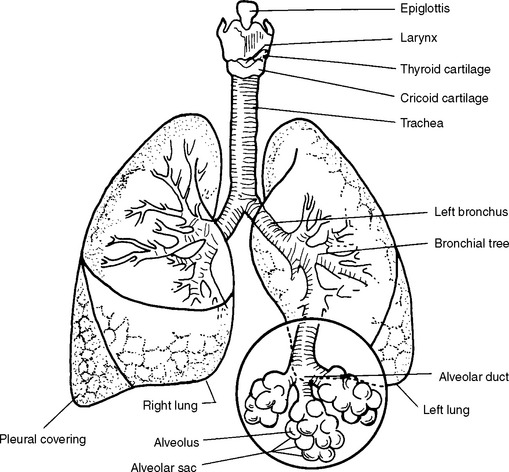
Many drugs employed during cardiothoracic surgery will impact the lung’s intrinsic mechanisms to match ventilation to perfusion matching either directly on hypoxic pulmonary vasoconstriction (HPV) or indirectly by altering cardiac output or vascular resistance. The compliance and resistance of the respiratory system will change during the course of surgery, especially those procedures requiring one-lung ventilation, and may necessitate frequent adjustments of the ventilator to optimize gas exchange and reduce lung injury. Dynamic influences of ventilatory pattern, posture, body habitus, agitation or pain, and inflammation can cause “air trapping” and drastically reduce alveolar ventilation. The anesthetic employed, both general and regional, will impact the control of respiration, reactivity of the airways, and the patient’s ability to maintain their airway, take a deep breath, and cough. The lung has ten (third generation airway) bronchopulmonary segments on the right and eight segments on the left that are readily identifiable by fiberoptic bronchoscopy (two segmental bronchi on the left are considered “fused”). Knowledge of the clinical anatomy and function of the respiratory system is essential for the safe, efficient, and appropriate perioperative management of intubation, mechanical ventilation, and anesthesia for the thoracic surgical patient.
